
Frustrated by repetitive or accidental urination every time while sneezing, coughing, or even exercising? Enfield Royal Clinic delivers superior Stress Urinary Incontinence in Dubai, specifically formulated to address compromised bladder or pelvic muscles’ impairment. Deploying FDA-authorized, evidence-supported strategies, our urologists or pelvic floor physiotherapists reduce unintentional urination and strengthen pelvic stability. Our innovative treatment plans are adapted in accordance with your requirements, facilitating you in reinstating strength and stability with enduring outcomes.
Quick Facts
💰 Cost: AED 180-AED 3500 each session.
⏱️ Duration: 30-60 minutes/ session.
✨Treatment Aims: Reduce bladder leaks, fortify pelvic floor muscles, and promote urinary management.
🛌 Downtime: Least, minor discomfort, urinary urgency, or brief inflammation for 1-2 weeks.
💪 Results Timeline: Initial improvements become obvious within 1-2 weeks, with optimal urinary control attained in 4-6 weeks.
👨⚕️ Who Performs It: DHA-certified gynecologists, urologists, or physiotherapists trained in pelvic floor therapy.
❌ Contraindications: Inappropriate for individuals with active UTI, intense pelvic organ displacement, or neurological concerns.
What is Stress Urinary Incontinence?
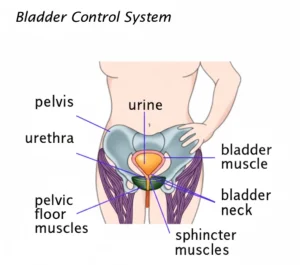
Stress Urinary Incontinence (SUI), also referred to as “stress incontinence,” is characterized by incidental urination when excessive strain is applied to the bladder from certain activities, caused by weakened pelvic floor muscles or the sphincter. It appears to be the most prevalent incontinence type, particularly in females. Its occurrence is linked with diminished urethral-bladder strength, allowing urine to escape while moments of increased abdominal pressure. It affects roughly 37% women along life’s course, and is rare in males. An individual might encounter minimal urination while engaging in specific activities like:
➺ Sneezing.
➺ Coughing.
➺ Laughing.
➺ Running.
➺ Hoisting weights.
➺ Jumping.
Types of Incontinence
It involves:
| Urinary Incontinence Type | Description |
|
Termed as “overactive bladder,” characterized by abrupt, intense urine urge that occasionally causes spontaneous leakage, specifically at nighttime. |
|
It involves repeated dribbling due to the bladder’s urine retention. |
|
Features pelvic muscles’ weakening post-delivery or tissue injury, resulting in leakage while conducting routine activities. |
|
Demonstrates restricted mobility or cognitive limitations that could delay prompt toilet accessibility. |
|
Integrates stress-associated and urge-linked indications, leading to leakage while exertion. |
|
An impaired sphincter post-prostate surgery might result in unplanned urine loss. |
Causes or Risk Factors
There exist several causes that trigger unintentional urination and are distinct in males and females, involving:
Women-Specific Causes
- Post-pregnancy, the pelvic muscles decline in strength, reducing the bladder-anchoring structures; hence, inducing leakage.
- Additionally, the period following menopause is marked by a significant drop in estrogen levels, diminishing tissue strength and lessening pelvic floor integrity.
- Urine-holding capacity gets noticeably compromised post-vaginal delivery or repeated deliveries, as they adversely affect pelvic musculature support.
- Excessive bodily weight stresses the bladder as well as the pelvic organs, leading to spontaneous urine escape.
Men-Specific Causes
- In males, the urethral muscles decline in strength following prostate surgery (prostatectomy), leading to trouble holding pee.
- Men’s capability of suppressing urination urge gets adversely impacted by the injured urinary sphincter due to its incomplete closure, enhancing the prospects of accidental urination.
- Also, the nerve trauma linked with prostate cancer contributes considerably by disrupting neurological pathways and regulating urine channels.
- Age-associated alterations in males reduce their sphincter’s integrity and bladder regulation.
Lifestyle & Other Causes
- The possibility of dribbling urine significantly elevates with excessive weight by putting unnecessary strain on the bladder.
- Intense lifting accompanied by vigorous bodily activities overworks pelvic muscles, resulting in urethral incontinence.
- Excessive caffeine as well as alcohol consumption leads to bladder irritation and intensifies stress-induced leakage.
- Additionally, diabetes, compromised posture, prolonged constipation, intimacy, and impaired core stability influence involuntary urine leak.
Symptoms
Stress Urinary Incontinence’s indications can be stratified into 3 levels, dictated by their severity grade:
| Grade 1: Mild
Urine escape, linked with certain activities, such as exertion, coughing, or sneezing, typically does not necessitate pads. |
Grade 2: Moderate
Undesired urine release in cases of lifting, running, or routine activities; pads might be required occasionally. |
Grade 3: Severe
Leakage associated with minor movements, such as bending or standing; pads are essential consistently. |
⚠️ Important: There exists a possibility that an individual might not leak while conducting these activities, while an action that is accredited with enhancing bladder strain might result in its provocation.
Benefits of Stress Continence Treatment
This treatment serves the positive aspects that involve:
1️⃣Improved Bladder Control
Its effective management assists an individual in regaining bladder management, notably lessening incidental urine leakage while carrying out routine activities.
2️⃣Enhanced Comfort & Hygiene
As treatment combats the consistent requirement for pad usage, it considerably hinders associated skin infections or irritation, hence encouraging personal ease and cleanliness practices.
3️⃣Guided Physical Movement
With restored bladder management, an individual is encouraged to engage in bodily activities as well as routine chores void of interruption or incontinence-associated fear.
4️⃣Improved Daily Life
Resolving stress incontinence facilitates individuals’ involvement in recreational, occupational as, as well as social activities with enhanced self-assurance, leading to entire well-being.
5️⃣Lessened Psychological Distress
By reducing frequent leakage and its effective regulation, an individual notices a significant decline in awkwardness, while fostering psych-social wellbeing.
Who is an Appropriate Candidate?
Living up with below-mentioned criterion might be an indication to seek treatment for peeing unexpectedly:
✔️Adults whose routine, occupational, and social activities are impacted by weak bladder control.
✔️Individuals observing a significant decline in their self-assurance and enhanced self-consciousness or distress as a result of incidental urine escape.
✔️People demonstrating willingness to comply with Kegel exercises, routine modifications, or clinical solutions.
✔️Persons possessing a stable clinical record.
Who might not be Suitable?
It is inadvisable for the following individuals to receive this treatment:
❌Children or adolescents due to their underdeveloped pelvic region.
❌Patients encountering critical clinical conditions that rule out surgical intervention or certain procedures.
❌People encountering prior Urinary tract infections (UTIs) or unregulated bladder concerns are required to address them with precedence.
❌those individuals demonstrating unwillingness to comply with postcare guidelines, directed exercises, or behavioural protocols.
Preparing for your Appointment
- You might be asked by your healthcare provider to hand in the required documentation regarding your stress incontinence indications.
- Also, it might be suggested to jot down your urination patterns, fluid consumption, and leaks in your bladder diary, intended at directing diagnosis and lessening requirement for additional testing.
- In case you require special testing, you can be referred to a urologist or female pelvic health specialist (urogynecologist) for your condition’s precise evaluation.
📝What you can do
To get benefitted at maximum from your appointment, you must observe the below mentioned guidelines:
- Accompany a loved one to reiterate the crucial details.
- Document your medical indications, vitamins, supplements, or medications along with their dosage schedule.
🩺Who can You Consult?
- Urogynecologist— a gynecologist having extensive training/ specialization in bladder and pelvic floor concerns.
- Gynecologist.
- Urologist— a surgeon possessing expertise in bladder or kidney complications.
How Doctors Diagnose Stress Incontinence
It initiates with the insightful review of the client’s clinical record and indications, along with physical assessment, which involves pelvic exam (for females) or rectal exam (for males), coupled with a concise neurological assessment. Several testing means can be utilized to spot its origin as well as intensity; these involve:
- Urinalysis– screening for indications of infections or blood traces in urine.
- Bladder ultrasound– measures bladder efficiency by assessing residual pee.
- Urodynamic study– examines bladder functionality, pelvic muscles’ integrity, and identifies incontinence’s type.
- Cystoscopy– employs a tiny scope for bladder and urethra analysis regarding structural concerns.
- Erect stress test– figures out pee leaks while coughing or standing.
- Urinary stress test– watches for leakage triggered by excessive strain on fila led-up bladder.
- Post-void residual measurement– investigates unvoided urine via an ultrasound or a catheter.
- Pressure-flow study– assesses bladder strength for complete drainage.
- Pad test– tracks pee leakage while routine activities.
- Uroflowmetry– checks out for peeing rate.
- Additional ultrasound– examines bladder capacity, bladder exit mobility, while ruling out gynecological concerns.
Management & Treatment Options
Its treatment is dependent on intensity, primary origins, and the patient’s preferences, and a structured approach is often suggested by the healthcare provider, commencing from conservative approaches and advancing to clinical devices or surgery, if essential.
01. Conservative & Lifestyle Management
- Pelvic Floor Exercises (Kegels): Enhance bladder or pelvic floor muscles via persistent practice across 3-6 months.
- Bladder Training: Timed urination to facilitate bladder regulation, particularly in cases of mixed incontinence.
- Biofeedback & Electrical Stimulation: Guided strategies to elevate pelvic muscle coordination and amplify Kegel efficiency.
- Lifestyle Adjustments: Encompasses weight maintenance, ceasing tobacco usage, restricting urine irritants, adequate fluid intake, and tackling persistent constipation or coughing.
02. Medical Devices
- Vaginal Inserts: Insertable, tampon-shaped instruments, providing brief assistance to the rethra while activities.
- Pessaries: Detachable vaginal tools that lifts bladder opening as well as the urethra, specifically in females. Entails routine cleansing.
03. Procedural & Surgical Interventions
| For Males | For Females |
|
|
What Should I Do After My Surgery for Urinary Incontinence?
1.Follow-Up & Monitoring
- As per your healthcare provider’s directions, schedule yearly clinical reviews and subsequent appointments.
- Promptly keep your healthcare specialist updated in cases of continued bleeding, pelvic ache, fluid secretions, or soreness while intercourse.
2.Questions & Guidance
- Communicate with your healthcare provider regarding supplementary queries or concerns linked with recovery, movement limitations, or consistent care.
3. Managing Complications or Concerns
- To explore treatment possibilities, review complications or atypical indications with your clinician.
- Receive a second perspective from a pelvic reconstruction specialist if you possess uncertainty regarding existing clinical guidance.
4.Special Considerations for Mesh Slings
- Disclosing your mesh sling’s positioning record to your healthcare provider specifically prior to potential pregnancies, operations, or clinical interventions.
How do you treat Stress Incontinence Naturally?
a.Routine Adjustments
- Trim extra pounds (≥30 BMI) to omit excessive bladder strain.
- Level up the consumption of fibre-packed meal options to ward off constipation.
b.Sex & Intimacy Tips
- Observe bladder emptiness prior to intercourse.
- Explore various sex positions that lessen leaks.
- Keep supplies (towels, pads) accessible.
c.Coping & Routine Life
- Ensure bringing spare clothes and absorbent pads.
- Familiarize yourself with restroom facilities.
- Practice skin’s thorough dryness and utilize barrier ointment, if required.
Stress Urinary Incontinence Cost in Dubai
Generally, the pricing bracket for Stress Urinary Incontinence commences from AED 180 and extends beyond AED 3500 each session. The final expenditure is affirmed post-analysing various aspects that involve the condition’s intensity, treatment approach, clinical competence, and individualized care requirements. A comprehensive expenses breakdown is listed below:
|
Treatment/ Session |
Approximate Cost |
|
Initial Consultation & Assessment |
AED 300 – AED 800 |
|
Laser or Minimally Invasive Procedure |
AED 2,000 – AED 6,500 |
|
Single Non-Surgical Pelvic Floor Therapy Session |
AED 300 – AED 800 |
|
Follow-Up / Maintenance Session |
AED 250 – AED 600 |
|
Customized |
AED 1,500 – AED 5,000+ |
Stop Leaks, Start Living with Effective Bladder Leak Treatment- Book Now!
Done with frequent leakage episodes and feeling at unease, particularly while socialising? Stress Urinary Incontinence at Enfield Royal Clinic is specifically formulated to tone up pelvic muscles, improve bladder management, and revive self-assurance. From non-invasive and least interventionist to innovative laser treatments, our DHA-licensed experts create an individualized treatment approach to align with your distinct requirements. Don’t permit urinary leaks to hold you back. Reserve your session straight away and embrace a path towards empowered, relaxed, and liberated you. Our staff guarantees 24/7 accessibility to address your queries and assist you throughout treatment.
FAQs
Is there any probability of stress incontinence escalating?
Surely! Nicotine intake and excessive bodily weight can worsen mild stress incontinence.
Can stress incontinence be addressed with certain medicational usage?
Though there does not exist an FDA-authorized drug, duloxetine might be utilised informally in certain cases.
Does stress urinary incontinence appear to be the enduring condition?
Periodically! Routine modifications, instruments, exercise patterns, or certain operational means can relieve or eliminate indications.
Is it considered typical to encounter urine escapes occasionally?
Yes, even periodic leakage while sneezing, coughing, etc are identified as stress incontinence.
Does this treatment encompass any sort of complications?
Yes, resembling any other operational intervention, but options such as bulking agents or slings are usually secure and effective.
Is seeking clinical assistance for a minor urination encouraged?
Yes! Instant regulation through exercising or routine adjustments can prevent intensification.
On average, what appears to be the pricing bracket for stress urinary incontinence?
While it is mainly dictated by the chosen approach, the condition’s intensity, and clinical standing, etc., AED 180-AED 3500 is viewed as its typical expenditure.
Dr. Sannia Awais
Dr. Sannia Awais has a wider experience in the field of Aesthetic Medicine, Hair restoration,... Dr. Hany Chidiac
Stay Younger Forever! Stay Young Forever From The Inside Out with our Anti Aging and... Dr Mahmoud Akrama
Dr. Mahmoud Akrama is a skilled general physician who specializes in aesthetic medicine and laser... Dr. Mahya Kanani
Dr. Mahya Kanani is a board-certified Obstetrician & Cosmetic Gynecologist. She is also DHA registered... Dr. Ahmed Naji Attiyah
We proudly announce yet another addition to the Enfield Royal Clinic family. Dr. Ahmed Naji... Dr. Diya Aldeen Mohammed
We are proud to announce the newest member and brilliant addition to Enfield Royal Clinics.... Dr Tamara Talib Hasan
Healthy smiles, and happy lives, Choose your path to oral wellness with our professional dentists-Dr... Dr. Nabaa A.Raheem
Redefine Your Beauty Standards With Expert Guided Treatments from Dr. Nabaa A. Raheem. Dr. Nabaa... Dr Rashah Al Ahmed
Eat smart, and live well—your journey to health starts here with our expert nutritionist and... Dr. Nagham Mohammed Karagholli
Dr. Nagham Mohammed Karagholli: Precision Surgery for a Healthier Tomorrow! A surgeon specializing in laparoscopic... Dr. Abdullah Hussam Mezel
Transform Your Smile with Precision and Expert Care – Dr. Abdullah Hussam Mezel. Dr. Abdullah... Dr.Nibras Sufeian AlDoori
Dr. Nibras Sufeian AlDoori: Where Family Care Meets Timeless Beauty! Dr. Nibras Sufeian is a... DR. Mohamad Sameer Alsalih
Radiant skin, confident you—discover your journey to flawless skin with Dr. Mohamad Sameer Alsalih. Dr.... Dr. Hani Al Mozawer
He is a leading urologist with over 05 years of experience, renowned for his expertise in... Dr Mohammad Abu Al-izz
Mohammad Abu Al-Izz — Understanding Minds, Transforming Lives DHA & DOH Licensed | Jordanian Board-Certified... Dr. Osama Shaheen
“Your smile deserves the best dentist, Dr. OSAMA SHAHEEN, who crafts Confident Smiles with Precision... Dr. Tamim Hasan
“Dr. Tamim Hasan– an experienced and expert dentist committed to delivering precise and compassionate dental... 






































































